Thyroid cancer specialist in Bareilly- Rohilkhand Cancer Institute | Pet CT Scan Centres in Bareilly

Thyroid cancer
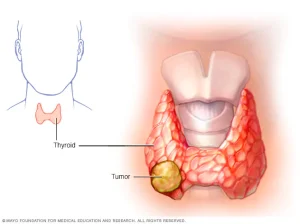
Thyroid cancer is a cell growth that begins in the thyroid. The thyroid gland is a butterfly-shaped gland in the base of the neck, directly below the Adam’s apple. Thyroid hormones control heart rate, blood pressure, body temperature, and weight.
Thyroid cancer may not exhibit any signs at first. However, when it grows, it can create signs and symptoms including as swelling in your neck, changes in your voice, and difficulty swallowing.
Thyroid cancer may not exhibit any signs at first. However, when it grows, it can create signs and symptoms including as swelling in your neck, changes in your voice, and difficulty swallowing.
Thyroid cancer appears to be on the rise.Improving imaging technology, which enables doctors to detect tiny thyroid malignancies on CT and MRI scans performed for other reasons (incidental thyroid cancers), could contribute to the rise. Thyroid tumours discovered in this manner are typically tiny and respond well to treatmentWhat are the warning signs of thyroid cancer? You or your healthcare provider might feel a lump or growth in your neck called a thyroid nodule.
Symptoms
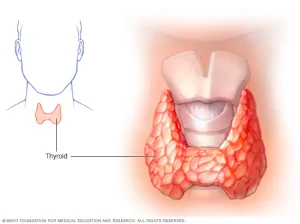
Most thyroid malignancies have no early warning signs or symptoms. As thyroid cancer progresses, it may result in:
A lump (nodule) that can be felt through your neck’s skin
A sense that close-fitting shirt collars are becoming overly restrictive
Changes in your voice, such as increased hoarseness
Having difficulty swallowing
Neck lymph nodes that are swollen
Neck and throat discomfort
When should you see a doctor?
Make an appointment with your health care provider if you see any signs or symptoms that concern you.
Causes
Thyroid cancer develops when cells in the thyroid undergo DNA alterations. The DNA of a cell includes the instructions that inform the cell what to do. The modifications, known as mutations, instruct the cells to grow and replicate rapidly. When healthy cells would normally perish, the cells continue to live. Cells clump together to create a mass known as a tumour.
The tumour might invade adjacent tissue and expand to the lymph nodes in the neck (metastasize). Cancer cells can sometimes move beyond the neck to the lungs, bones, and other regions of the body.
It is unclear what causes the DNA alterations that cause thyroid cancer in the majority of cases.
Types of thyroid cancer
Doctors classify thyroid cancer based on the types of cells found in the tumor. They examine a sample of tissue from your cancer under a microscope to determine its type. The type of thyroid cancer you have influences your therapy and prognosis.
Thyroid cancer comes in several forms, including:
The Thyroid malignancies that have been differentiated. Thyroid cancers that begin in the cells that create and store thyroid hormones fall into this broad category. These are known as follicular cells. When seen through a microscope, differentiated thyroid cancer cells resemble healthy cells.
Papillary
Thyroid cancer of papillary form. Thyroid cancer is the most prevalent form. It can arise at any age, although it most commonly affects persons between the ages of 30 and 50. Even if the cancer cells extend to the lymph nodes in the neck, most papillary thyroid tumours are tiny and respond well to treatment. A small percentage of papillary thyroid cancers are aggressive and may spread to other parts of the body or involve tissues in the neck.
Follicular
Thyroid cancer with follicular cells. This uncommon kind of thyroid cancer typically affects adults over the age of 50. Cells from follicular thyroid carcinoma seldom travel to the lymph nodes in the neck. Some large and aggressive malignancies, on the other hand, may spread to other regions of the body. Most follicular thyroid cancers move to the lungs and bones.
Hurthle
Thyroid cancer of the Hurthle cell type. This rare kind of thyroid cancer was previously classified as follicular thyroid carcinoma. Because cancer cells act differently and respond to different therapies, it is now considered a distinct kind. Hurthle cell thyroid tumours are aggressive and can spread to other parts of the body after involving structures in the neck.
Thyroid cancer with poor differentiation. This uncommon kind of thyroid cancer is more aggressive than other differentiated thyroid tumours and frequently fails to respond to standard therapies.
Anaplastic
Thyroid cancer that is anaplastic. This uncommon kind of thyroid cancer spreads swiftly and is difficult to treat. Treatments, on the other hand, can help halt the progression of the condition. Anaplastic thyroid carcinoma is more common in adults over the age of 60. It can cause severe signs and symptoms, such as neck swelling that develops quickly and can lead to breathing and swallowing difficulties.
Medulla
Thyroid carcinoma in the medulla. This uncommon kind of thyroid cancer develops in C cells, which generate the hormone calcitonin. Elevated calcitonin levels in the blood can suggest medullary thyroid carcinoma at an early stage. Some medullary thyroid tumours are caused by the RET gene, which is passed down from parents to children. Changes in the RET gene can result in familial medullary thyroid cancer and type 2 multiple endocrine neoplasia. Thyroid cancer risk is increased in families with medullary thyroid carcinoma. Type 2 multiple endocrine neoplasia raises the chance of thyroid cancer, adrenal gland cancer, and other cancers.
Other uncommon types. Other, extremely rare kinds of cancer can begin in the thyroid. Thyroid lymphoma, which develops in thyroid immune system cells, and thyroid sarcoma, which begins in thyroid connective tissue cells, are two examples.
Risk factors
The following factors may raise the risk of thyroid cancer:
Female gender. Thyroid cancer affects women more frequently than males. Experts believe it is related to the hormone oestrogen. People who are born with the female sex have higher levels of oestrogen in their bodies.
People who are assigned feminine sex at birth have higher levels of oestrogen in their systems.
Certain genetic syndromes are inherited. Familial medullary thyroid cancer, multiple endocrine neoplasia, Cowden syndrome, and familial adenomatous polyposis are all genetic syndromes that increase the risk of thyroid cancer. Medullary thyroid cancer and papillary thyroid cancer are two types of thyroid cancer that can run in families.
Complications
Thyroid cancer that comes back
Thyroid cancer can recur despite effective therapy, and it can even happen after the removal of your thyroid if cancer cells have spread outside of the thyroid before removal.
Most thyroid cancers, including the most common forms — papillary thyroid cancer and follicular thyroid cancer — are unlikely to recur. Based on the specifics of your cancer, your health care practitioner can tell you if it has an elevated risk of reoccurring.
If your cancer is aggressive or spreads outside your thyroid, recurrence is more likely. When thyroid cancer recurs, it is usually discovered within the first five years of your first diagnosis.
Thyroid cancer may recur in:
- Lymph nodes in the neck
- Small pieces of thyroid tissue left behind during surgery
- Other areas of the body, such as the lungs and bone
Your doctor may recommend periodic blood tests or thyroid scans to check for symptoms indicating the return of your cancer. During these encounters, your provider may inquire if you’ve had any signs or symptoms of thyroid cancer recurrence, such as:
- Neck pain
- A lump in the neck
- Trouble swallowing
- Voice changes, such as hoarseness
Cancer of the thyroid that spreads (metastasizes)
Thyroid cancer can spread to surrounding lymph nodes or to other regions of the body at times. Cancer cells that spread may be discovered when you are first diagnosed, or they may be discovered after treatment. The vast majority of thyroid tumours never progress.
When thyroid cancer spreads, it usually goes to:
Lymph nodes in the neck
Lungs
Bones
Brain
Liver
Skin
When you are first diagnosed with thyroid cancer, imaging tests such as CT and MRI may reveal spread. Following successful treatment, your doctor may advise you to schedule follow-up sessions to look for evidence that your thyroid cancer has spread. These consultations may include nuclear imaging scans, which use a radioactive type of iodine and a specific camera to detect thyroid cancer cells.















