What is carcinoma?

Cancer that develops in epithelial tissue is called a carcinoma. The majority of your organs, as well as your skin and internal body pathways like your oesophagus, are lined with epithelial tissue. The majority of malignancies that affect your head and neck, skin, breasts, kidney, liver, lungs, pancreas, and prostate gland are carcinomas.
Carcinoma makes for 80% to 90% of all cancer diagnoses, making it the most prevalent type of cancer. Epithelial tissue, which lines your organs, internal body passages, and skin, is where cancerous tumours develop. Tumours known as carcinoma can develop on your skin, in your lungs, breasts, prostate, colon, kidneys, pancreas, and other organs.
Most people categorise cancer according to where it develops (colorectal cancer, breast cancer, etc.), although this is merely one method. In addition, the types of tissues where cancer cells first develop are used by scientists to classify various malignancies.
The following tissue types are used to classify cancer:
Carcinoma
Epithelial tissue is where cancer begins.
Myeloma
Plasma cells in the bone marrow are where cancer begins.
Leukemia
The bone marrow, which produces blood cells, is where cancer first develops.
Lymphoma
The bone marrow, which produces blood cells, is where cancer first develops.
Sarcoma
Cancer starts in connective and supportive tissue (ex., muscle, bone, cartilage, etc.).
Mixed types
Many different tissue types can become cancerous.
How is cancer categorised based on its spread?
Tumours are solid masses that are created by the growth and multiplication of cancer cells. Cancerous cells can separate from tumours and “metastasize,” or spread to different regions of the body. How far a cancer has spread is indicated by its label.
Carcinoma in situ: The carcinoma hasn’t spread.
Invasivecarcinoma:In close proximity to where it originated, the cancer has progressed to adjacent tissue. In close proximity to where it originated, the cancer has progressed to adjacent tissue.
Metastatic carcinoma: Your body now has other areas where the cancer has spread.
What kinds of carcinoma are there?
Carcinomas are a broad category of cancers. The following are some of the most typical carcinoma types:
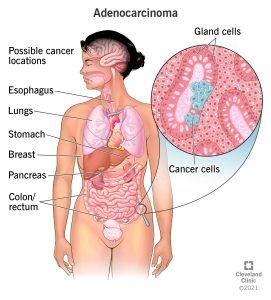
Adenocarcinoma: begins in the glands that line the glands that coat your organs. Glandular epithelial cells release fluids including mucus and digestive juices. Adenocarcinomas make up the majority of cases of pancreatic, breast, colorectal, prostate, and adenocarcinomas. Renal cell carcinoma (RCC), an adenocarcinoma, is the primary cause of kidney cancer in 85% of cases. Hepatocellular carcinoma (HCC), an adenocarcinoma, is the most common type of liver cancer.begins in the glands that line the glands that coat your organs. Glandular epithelial cells release fluids including mucus and digestive juices. Adenocarcinomas make up the majority of cases of pancreatic, breast, colorectal, prostate, and adenocarcinomas. Renal cell carcinoma (RCC), an adenocarcinoma, is the primary cause of kidney cancer in 85% of cases. Hepatocellular carcinoma (HCC), an adenocarcinoma, is the most common type of liver cancer.
Basal cell carcinoma:The basal cell layer of your epidermis is where (BCC) begins. Your skin’s epidermis is the outermost layer. Your epidermis’ base is lined by a layer of basal cells. When the squamous cells at the top of your epidermis die, these cells take their place. Skin cancer of the most prevalent form is basal cell carcinoma.
Carcinoma of the skin cell :(SCC) begins in the squamous cell layer (top layer) of your epidermis. It typically manifests on your face, ears, neck, arms, legs, and other areas of skin that are exposed to the sun the most. The mucous membranes lining your lungs, oesophagus, head, and neck can also develop SCC. The second most typical kind of skin cancer is it. In general, basal cell carcinoma spreads more slowly than squamous cell cancer.
Ductal carcinoma in situ (DCIS) : begins in the milk ducts of your breast. Milk flows through your milk ducts and to your nipple during breastfeeding (chestfeeding). A carcinoma is said to be “in situ” if it hasn’t spread to cells outside of your milk ducts. DCIS is a type of breast cancer that is largely curable and is regarded as benign or preinvasive.
Invasive (infiltrating) ductal carcinoma starts in your breast milk ducts, like DCIS. Invasive ductal carcinoma, as opposed to DCIS, has spread to adjacent tissue. If left untreated, it could travel via your bloodstream and lymphatic system to other parts of your body. The most typical kind of breast cancer is it.begins in the milk ducts of your breast. Milk flows through your milk ducts and to your nipple during breastfeeding (chestfeeding). A carcinoma is said to be “in situ” if it hasn’t spread to cells outside of your milk ducts. DCIS is a type of breast cancer that is largely curable and is regarded as benign or preinvasive.
Invasive (infiltrating) ductal carcinoma starts in your breast milk ducts, like DCIS. Invasive ductal carcinoma, as opposed to DCIS, has spread to adjacent tissue. If left untreated, it could travel via your bloodstream and lymphatic system to other parts of your body. The most typical kind of breast cancer is it.
Who gets carcinoma?
Your risk of acquiring carcinoma may be influenced by specific demographic factors.
Age :If you’re 65 or older, your risk of developing carcinoma rises. Children rarely develop cancer.
Sex: The risk of developing carcinoma is higher in those whose gender at birth is designated male, with the exception of breast cancers.
Race/Ethnicity: By type of carcinoma, risks based on race differ. Black people are more likely to get some adenocarcinomas, such as lung, colon, and prostate cancer. The highest risk group for colon cancer is those who are Jewish and of Ashkenazi heritage. White persons and those with less melanin have a higher chance of developing skin-related carcinomas.
How common is carcinoma?
The majority of cancer diagnoses, between 80% and 90%, are for carcinoma.
What causes carcinoma?
Like all cancers, carcinoma develops when a genetic alteration turns a normally healthy cell into a malignant cell. That cancer cell continues to grow and produce additional cancer cells. The cancer cells might infect neighbouring healthy tissue if left untreated. The cancer cells may eventually spread (metastasize) through your lymphatic or blood systems to infiltrate other regions of your body.
Scientists are unsure of what triggers the mutation that results in cancer, although some circumstances may make you more susceptible.
What are the risk factors for carcinoma?
Depending on the specific form of carcinoma, different risk factors apply.
Adenocarcinoma
A risk of Since adenocarcinomas can develop in a variety of organs, including your breast, prostate, pancreas, oesophagus, colon/rectum, stomach, lungs, etc., risk factors for these cancers are extremely diverse. Typical risk elements include :Since adenocarcinomas can develop in a variety of organs, including the breast, prostate, pancreas, oesophagus, colon/rectum, stomach, lungs, etc., there are many different forms of adenocarcinomas. Typical risk elements include:
Tobacco use.
Drinking alcohol
Exposure to harmful toxins
Previous radiation therapy.
Genetic mutations such as BRCA, HNPCC, FAP, etc.
Squamous and basal cell cancer
Excessive exposure to UV radiation (from the sun or tanning beds).
Light-colored skin that burns or freckles easily.
Blue or green eyes, blonde or red hair.
An infection with a high-risk strain of HPV.
Previous radiation therapy.
Exposure to harmful toxins.
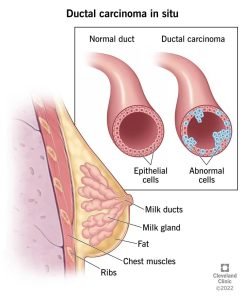
Developing malignant cells in the milk ducts of the breast.
Invasive and in situ ductal carcinoma
Breast cancer runs in the family, especially in younger relatives.
Genes for BRCA1 and BRCA2 that have undergone mutations.
A high BMI (at least overweight status).
Never having children or having reached maternal age.
Early onset of your first period.
Late menopause
How is cancer identified?
To determine variables that could raise your risk of carcinoma, your doctor will evaluate your family medical history and conduct a complete medical history. You’ll be questioned about your symptoms. If your doctor suspects you have carcinoma, they may suggest one or more of the following tests or procedures.
exam of the body. Your doctor will check for skin alterations that could be basal or squamous cell carcinomas. Breast exams enable your doctor to spot abnormal growths or symptoms, such as skin changes or nipple discharge, that could indicate ductal carcinoma.
a blood test. Protein levels, enzyme levels, tumour markers, and other signs can be found in blood tests and may help your doctor make a more accurate diagnosis.
Imaging. Mammograms and colonoscopies, which are common imaging procedures, can aid in the early detection of cancer. Imaging can also assist your doctor in narrowing down a diagnosis or determining whether your cancer has spread. Ultrasounds, mammograms, MRIs, CT scans, PET scans, and X-rays are examples of imaging procedures. To find tumours affecting particular organs, your doctor could suggest specialised imaging tests.
Biopsy. The only way to confirm a diagnosis of cancer is by a biopsy. Shave, punch, fine-needle aspiration, core needle, surgical lymph node, incisional, and excisional biopsies are among the procedures used to identify cancer. Despite variations in technique, all biopsies entail your doctor extracting tissue that is then examined for cancer cells in a lab.
How are cancers staged?
Cancer staging is a crucial aspect of diagnosis. The staging process enables your healthcare professional to record the size, lymph node spread, and distant spread of a tumour. Additionally, it offers crucial details about its dissemination.
Stage 0: The cancer has not spread beyond where it started. Stage 0 cancer is in situ and is often cured with prompt treatment.
Stage 1: The tumor is more obvious than in stage 0. The cancer has not spread to nearby tissues, organs, or lymph nodes.
Stage 2: The tumor is larger than stage 1 and may or may not have spread to your lymph nodes
.Stage 3: The tumor is large and has spread to nearby tissues or lymph nodes.
Stage 4: The cancer is metastatic, which means it has spread to other organs or parts of your body. step 0: kainsar jahaan banaStage 0: The cancer has not spread beyond where it started.
How is carcinoma treated?
Treatment for cancer is based on a number of variables, including your general health, the tumor’s stage, the specifics of the biopsy report, including pathology, your age, and your treatment goals. With you, your physician will go over a care plan that fits your particular circumstances.
Surgery: For safety reasons, your doctor could remove the tumour or cancerous cells together with any nearby healthy tissue. If the cancer is contained to one region and has not spread, they might advise surgery.
Chemotherapy: You may be given medications that either eliminate cancer cells or stop them from proliferating. Chemotherapy may be used in conjunction with procedures like radiation or surgery. Neoadjuvant chemotherapy can be used to reduce cancer cells prior to surgery so they are simpler to remove. Adjuvant chemotherapy can be used to treat cancer after it has already spread.
Radiation therapy: Radiation uses focused energy beams, such as X-rays, to either kill or stop the growth of cancer cells. It is frequently used in conjunction with chemotherapy and surgery. Radiation can be used to reduce a tumour before surgery or to eradicate any leftover cancer cells thereafter, similarly to chemotherapy. Depending on the type of carcinoma, radiation may also assist in the relief of symptoms.
Drugs that specifically target flaws or genetic alterations in cancer cells are used in targeted therapy. By focusing on these vulnerabilities, targeted therapy can either kill the cancer cells or stop them from proliferating.
Immunotherapy: Immunotherapy aids in the detection and destruction of cancer cells by the immune system. Along with other therapies like chemotherapy, your doctor might advise immunotherapy.
Hormone therapy: Reducing the levels of specific sex hormones in your body can inhibit the formation of cancer. For instance, prolonged oestrogen exposure has been associated with an increased risk of breast cancer. Prostate cancer has been connected to androgen exposure. Hormone therapy can reduce the effects these hormones have on the development of cancer.
Treatment may be curative, palliative, or a combination of the two, depending on your diagnosis. Remission is the aim of curative treatment. The term “complete cancer remission” refers to the absence of all signs and symptoms of the disease. You can better control your cancer symptoms with palliative care. As you navigate life after receiving a cancer diagnosis, it may also give you the confidence and comfort to feel more in control of your medical decisions.
How can I lower my risk of developing cancer?
Knowing potential risk factors and sharing them with your provider will assist. Consider the scenario where a close relative was diagnosed with breast cancer. Your doctor might then advise early screenings or more frequent breast exams. They could advise genetic testing to discover if you have any gene alterations that could raise your risk of developing cancer.
Certain lifestyle choices can lower your risk of developing certain types of carcinoma.
Do not smoke or use tobacco products.
Maintain a healthy body weight.
Limit your alcohol intake.
Use a sunscreen with SPF 15 or higher,
depending on how long you’ll be outside.
If possible, avoid being in the sun from 10 am to 4 pm.
Avoid tanning beds.